In the second week of October 2014 we distributed a survey to all patents receiving treatment at one of the Mandometer clinics in Sweden. The week was chosen at random.
The response rate was 80%, which was slightly higher than in 2013 (77%) and 2012 (70%). The results suggested that the patients who responded to the survey in 2014 were more severely ill than the patients who responded to the survey in 2013. Anorexia nervosa remained the dominant self reported diagnosis at 50%, up from 42% in 2013.
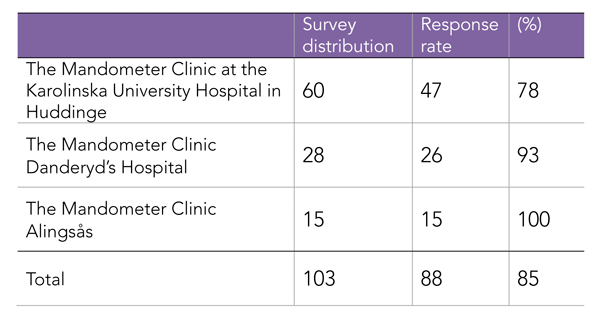
The majority of patients learned about Mandometer treatment through primary health care professionals (39%). This is surprising given the increasing proportion of visitors to the website (over 100,000 per year), yet only 12% state they learned about Mandometer treatment via the Internet. Patient satisfaction with treatment and the attitude of staff remained high (8.1 of out 10), and 83% of patients reported they would recommend Mandometer treatment to others. Of the 103 patients receiving the survey, 85% completed it.
Table 1. Survey distribution and response rate per clinic
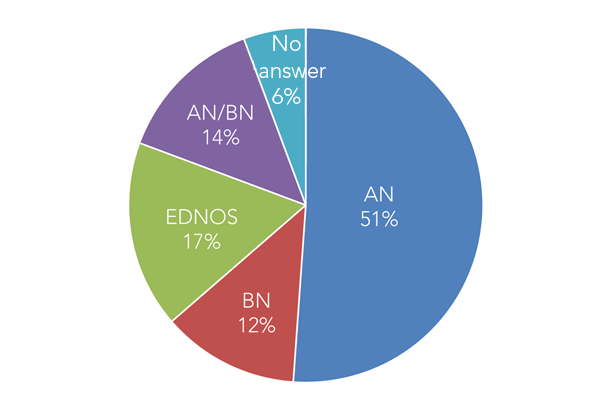
The patients surveyed had been in treatment for an average of 7.5 months (0.2-36 month range). There was a discrepancy between self diagnosis and clinician diagnoses (figure 1). Patients diagnosed with EDNOS by clinicians, frequently perceived themselves as having anorexia nervosa or bulimia nervosa, most likely due to having an anorexic weight or exhibiting bulimic behaviours, respectively.
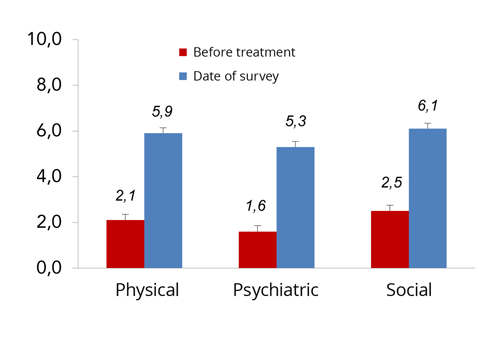
The graph below (figure 2) compares patient reports of physical, psychiatric and social wellbeing at the start of treatment to the time of being surveyed. Where 0=very poor and 10=Very good, the averages at they time of being surveyed were; physical (5.9), psychiatric (5.3) and social (6.1) wellbeing, compared to; physical (2.1), psychiatric (1.6) and social (2.5) wellbeing at the beginning of treatment.
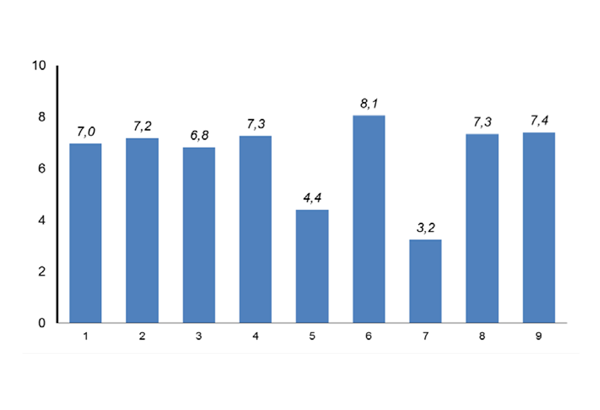
- How does the Mandometer treatment work?
- How familiar are you with the treatment?
- Have you been given information about treatment results?
- Do you feel involved in your treatment?
- How does our treatment compare to other treatment you have tried?
- How friendly do you find the staff at the Mandometer clinic?
- How satisfied were you with previous eating disorder treatment you received?
- How satisfied are you with Mandometer treatment?
- How does your experience of Mandometer treatment compare to your experience of previous treatments?
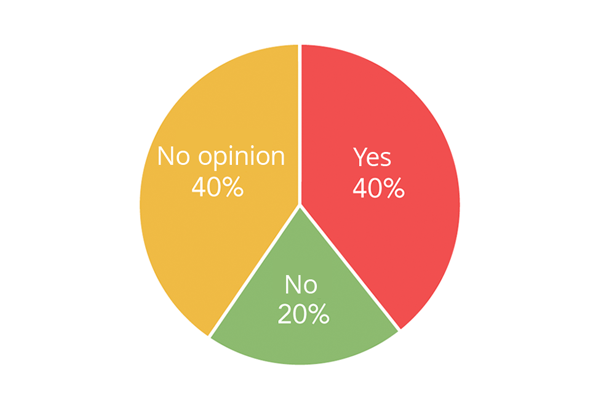
34 out of 35 patients who felt that something was missing from Mandometer treatment suggested one or more of the following improvements:
- Meet with patients who are in remission
- Learn more about how the body works
- Speak with a psychologist
- Shorter waiting times for starting treatment
- Movie room
- Participating in cooking
- A more modern Mandometer!
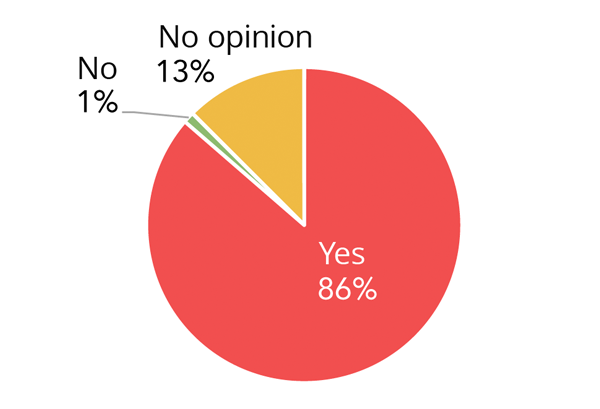
Eighty-six percent of patients responded that they would recommend Mandometer treatment to a friend with an eating disorder (Figure 5).



