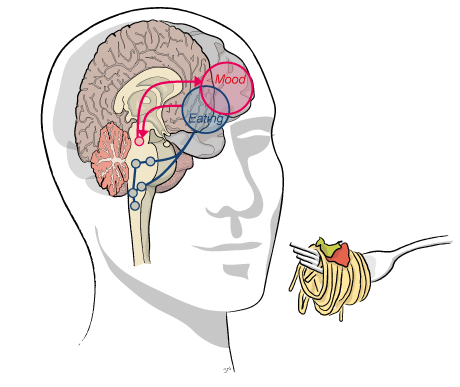
It is important to change behaviour:
Normalising food intake, eating behaviour, activity levels, and sleep patterns provide the foundations for retuning activities of normal daily living. It is through restoration of these behaviours that one is able to return to school, work, socialising and leisure activities.
Patients learn to eat and identify signals of hunger and satiety by training to eat with the Mandometer®. Following meals, patients rest in a heated environment (warm room, heat blankets) to reduce the need to compensate for eating with physical activity, and to decrease anxiety. Patients who are underweight are always cold, and normal weight patients with bulimia nervosa are generally cold when they are not binge-eating. With time, patients learn to become comfortable with resting in heat and often fall asleep. As growth hormone is produced during sleep, this is particularly important for patients who have stopped growing due to starvation, but still have the potential to grow taller. Each patient is assigned a personal case manager who works intensively with the patient to build their confidence and motivate them towards recovery. Patients gain confidence which each step forward they take. Our case managers are very experienced and have the skills to handle any negative thoughts that may arise.
Our treatment is based on scientific studies.
Thoughts or cognitions are driven by behaviour not the reverse. If you are uneasy or anxious about a particular situation, it is likely you will avoid that situation. Other similar situations may also trigger anxiety. As patients gradually face their anxiety surrounding food, the thoughts that have been maintaining their disturbed eating behaviour begin to have less power. Progress is enhanced with a positive reward; as eating behaviour normalises, anxiety decrease and thoughts become normal.
Modjtaba Zandian, researcher at the Karolinska Institute and Quality Assurance at AB Mando (Mando).

Normalising eating behaviour
Each patient is given an individualised meal plan and provided with a Mandometer; a medical device that is used in treatment to teach patients how to eat and to recognise signals of hunger and satiety. The Mandometer is used at meals every day until eating behaviour normalises. It usually takes 3-4 months.
Our method of treatment is to normalise eating behaviour. This includes being able to sit at a table with others and eat a meal. We train our patients to change their behaviour in successive steps. For example, a patient may set the table but does not eat, a patient may fill a glass with water but does not drink, or a patient may put food on their plate but not eat any of the food on their plate. This is done until the patient takes their first bite of food. Training of eating behaviour is determined on an individual basis. I have seen patients who were unable to eat when they started treatment, eating in the dining room with others after only a few days of being here with us.
Modjtaba Zandian, researcher at the Karolinska Institute and Quality Assurance at Mando.
The mindset relating to food and weight is the same for all patients. Patients are afraid of gaining weight, but at the same time are obsessed with food. The conflict between eating and not eating dominates the patient’s thoughts all day long, regardless of age and gender. The contradiction in the conflict is that you eat nothing at all or you binge-eat, because food is simultaneously forbidden and desirable. A patient who is afraid of gaining weight is on a quest lose weight, no matter how much the patient weighs. It does not matter if weight is 27 or 87 kg, because weight gain is always feared. The fear and anxiety experienced by the patient give them an unrealistic and negative body image, leading to thoughts that the body and food intake must be combatted and mastered. When treating a patient with anorexia nervosa, it insufficient to just teach them to eat; you must also teach the patient to stop eating, because the alternative to not eat is to binge-eat. This is something that myself and other clinicians must take responsibility for. This is often lacking in treatment.
(from conversations with Clinical Psychologist Sven Holmgren, Hetsätarna, Författarförlaget Stockholm 1984).

Heat and Rest
Heat has a relaxing and anti-anxiety (anxiolytic) effect, and helps patients relax and keep still without becoming overwhelmed with anxiety. Patients feel most compelled to move before meals (in order to allow themselves to eat), and after meals (to compensate for the food they just ate). Resting is very important because it encourages the patient to refrain from compensatory/compulsive activity, and teaches patients to sit with their anxiety and challenge the eating disorder thoughts as they arise.
The warm rooms at our Mandometer Clinics are decorated like small bedrooms with a comfortable bed to give the patient a warm and cozy feeling. Patients can self-regulate the heat up to 40° C (F 104). We also provide our patients with heat blankets and jackets.
It’s great to rest. It’s the best thing about this place. It’s glorious to lie in a warm room. Sometimes you are very cold after eating. So it’s a brilliant idea.
Sofie, 26 years old from Australia.

Decreasing physical activity
People with eating disorders are typically very physically active. This decreases food intake and body weight, but might increase body temperature: Most patients with anorexia nervosa are women, and women feel cold at all times when eating only little food. Men do not because they generate more heat; their body surface area is smaller than that of women in relation to body mass that generates the heat. It is very important to reduce physical activity in order to increase body weight and to stop binge eating and vomiting. A very high level of physical activity can prevent weight gain as much as disordered eating can, as well as impair heart function and weaken bones. It can even be life threatening.
Physical activity is therefore reduced early on in treatment, to be gradually reintroduced and eventually restored to normal as health is regained.

Social reconstruction
In addition to attending to our patients’ nutritional needs and eating behaviour we help them accept and appreciate their bodies, understand the mechanisms underlying eating disorders and recognise warning signals, develop emotional regulation, and eventually, return to school or work. The treatment also focuses on improving self esteem and self awareness, building confidence and enjoyment, and managing social situations and interpersonal relationships.
Each patient works with their case manager to set up short term goals, such as visiting a friend or reading a book, and long term goals, such as going on a holiday or learning to drive. A structured plan, for returning to school or work, is arranged with the patient. We encourage our patients to resume social activities, such as meeting with friends, going to parties, or taking a summer job or volunteer role.
As patients reach their goals their confidence increases, and in many cases a patient’s confidence is better after Mandometer treatment than it was prior to becoming ill.